Volume 2, Issue 1, Orginal Rearch Article – Dec 27, 2025, Pages 37-43,
DOI: 10.64951/jmdnt.2026.1.04
Does Surgical Sequencing Still Matter in Fully Digital Bimaxillary Orthognathic Surgery? A Retrospective Accuracy Study of 46 PSI‑Guided Cases
Ayhan Yildirim¹, René Hertach², Vedat Yildirim¹
¹ Hochschule Zurich, Department of Medicine, Albisstrasse 80, 8038 Zurich, Switzerland
² Hochschule Zurich, Department of Dentistry, Albisstrasse 80, 8038 Zurich, Switzerland
Received: 08 June 2025, Revised: 21 October 2025, Accepted: 16 November 2025, Available online: 07 December 2025, Version of Record: 27 December 2025
© 2025 Journal of Medicine and Dentistry (JMDNT)
This article is published under the Creative Commons Attribution 4.0 International (CC BY 4.0) License.
You are free to share and adapt the material for any purpose, even commercially, as long as proper credit is given to the original author(s) and source.
Full license details
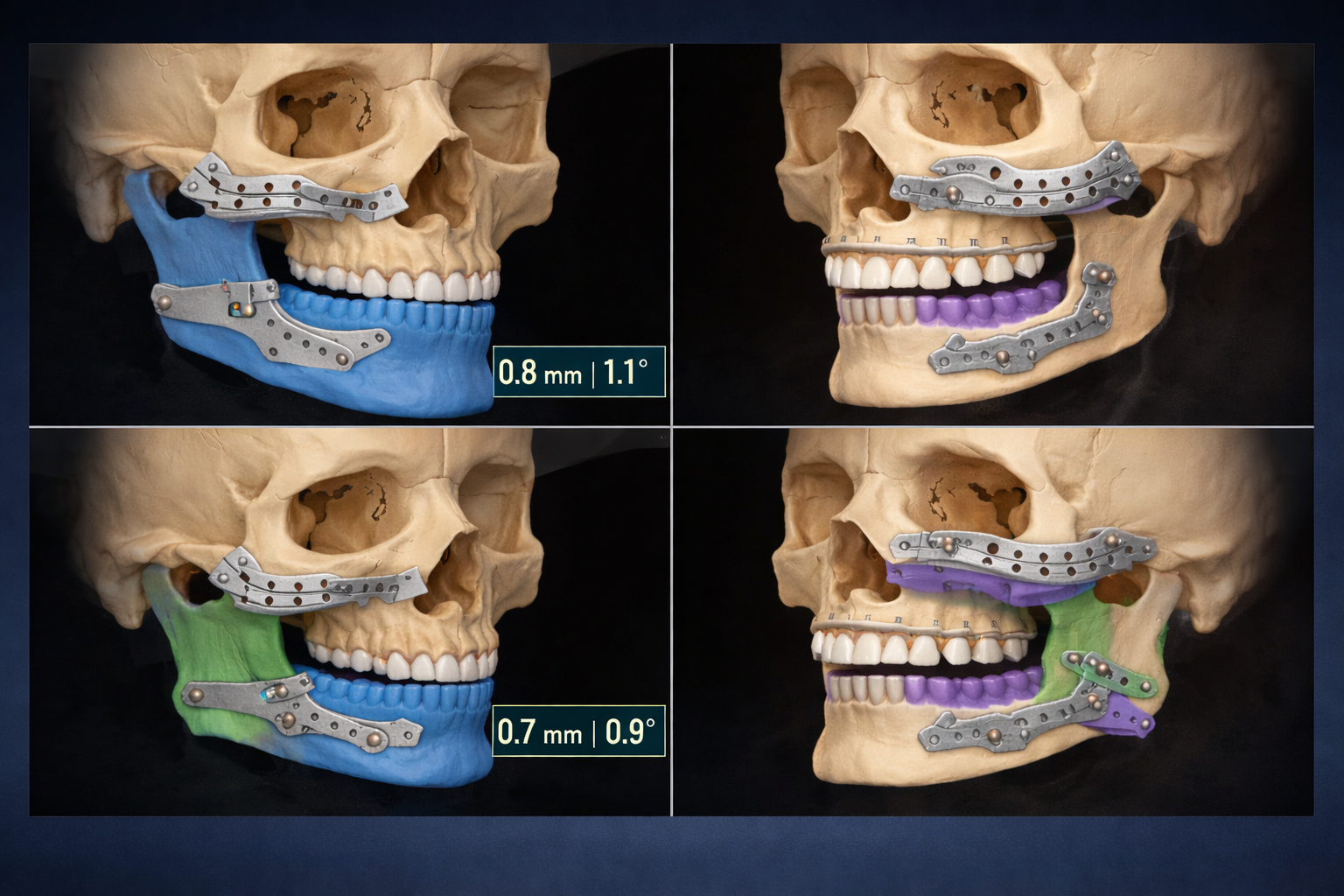
Screenshot of the patient-specific implant (PSI) planning interface showing four views of the maxilla and mandible in bimaxillary orthognathic surgery. Each quadrant illustrates 3D models of the skeletal structures with digitally designed implants and color-coded segments. The lower left measurement frame has been standardized to black. This visualization represents the virtual surgical planning (VSP) workflow used to ensure precise osteotomy and fixation placement prior to surgery – Seeklinik Zurich, Specialized Clinic for Oral, Maxillofacial and Plastic Facial Surgery, Zurich, Switzerland.
ABSTRACT
Background: The optimal sequence in bimaxillary orthognathic surgery (maxilla‑first vs mandible‑first) has long been debated. The advent of virtual surgical planning (VSP) and patient‑specific implants (PSI) has improved spatial control and precision, potentially diminishing the impact of sequencing.
Objective: To evaluate whether sequencing influences surgical accuracy in fully digital PSI‑guided bimaxillary surgery.
Methods: A retrospective cohort of 46 consecutive patients who underwent bimaxillary orthognathic surgery with VSP and PSI was analyzed. Surgical sequence (mandible‑first: n=22; maxilla‑first: n=24) was selected based on clinical indication. Postoperative CBCT (≤4 weeks) was superimposed on the VSP to assess translational and rotational deviations. Clinically acceptable accuracy was defined as ≤2 mm and ≤2°.
Results: Both sequencing approaches achieved high accuracy for maxillary and mandibular positioning. Mean translational and rotational deviations were within predefined clinical limits. No significant differences were noted between sequencing groups. No case required conversion from PSI-guided to splint-based transfer.
Conclusions: In fully digital, PSI‑guided workflows, surgical sequence appears secondary to planning precision and fixation strategy. Both mandible‑first and maxilla‑first approaches can achieve high surgical accuracy when selected based on clinical indications.
Keywords: orthognathic surgery; surgical sequencing; virtual surgical planning; patient‑specific implants; surgical accuracy
1. INTRODUCTION
Bimaxillary orthognathic surgery is widely used for the correction of dentoskeletal deformities, addressing both functional occlusion and facial aesthetics. Historically, the choice of surgical sequence (maxilla‑first vs mandible‑first) was dictated by intraoperative stability. Conventional wire fixation favored a maxilla‑first approach, as the maxilla could serve as a stable reference for mandibular repositioning [1]. The introduction of rigid internal fixation, PSI, and VSP has enabled surgeons to consider the mandible‑first sequence without compromising accuracy [2–4].
Virtual surgical planning (VSP) allows preoperative simulation of osteotomies, jaw movements, and splint or PSI design, enhancing predictability. Patient-specific implants (PSI) further improve accuracy by translating the digital plan directly to the patient [3,5]. Despite these technological advances, the relevance of sequencing remains debated. Systematic reviews report no definitive superiority of either sequence, emphasizing that sequencing should be based on clinical indications rather than convention [1,2].
This study aims to evaluate the influence of sequencing on surgical accuracy in fully digital, PSI-guided bimaxillary surgery. We hypothesized that sequencing does not significantly impact postoperative accuracy when VSP and PSI are employed.
2. MATERIAL AND METHODS
Study Design and Patients
This retrospective study included 46 consecutive patients undergoing bimaxillary orthognathic surgery (Le Fort I osteotomy and bilateral sagittal split osteotomy). The study was conducted at the Seeklinik Zurich, Specialized Clinic for Oral, Maxillofacial and Plastic Facial Surgery, Zurich, Switzerland. All surgeries were performed by the same experienced surgeon to minimize inter-operator variability and ensure consistency in technique and outcomes. The cohort consisted of 22 patients undergoing mandible-first sequencing and 24 undergoing maxilla-first sequencing. All patients underwent preoperative virtual surgical planning (VSP) and received patient-specific implants (PSI), including cutting guides and fixation plates. Backup occlusal splints were fabricated as a contingency in case of PSI placement difficulties, but none were required. Postoperative CBCT was obtained within 4 weeks for all patients.
Virtual Planning and PSI Fabrication
Preoperative VSP defined targeted maxillary and mandibular positions, including translational and rotational movements. PSI were designed to guide osteotomies and fixation accurately, including cutting guides and patient-specific plates. Backup splints were prepared to serve as intraoperative safety measures in case of PSI placement difficulties; no patient required their use.
Surgical Procedure and Sequencing
Sequence selection was guided by clinical indications:
-
Mandible-first: preferred in counter-clockwise rotations, cleft patients, or multi-segmental maxillary osteotomies.
-
Maxilla-first: indicated for clockwise rotations, single-piece Le Fort I osteotomies, or limited fixation scenarios [1,6,7].
All surgeries were performed by the same surgeon to minimize variability.
Postoperative Accuracy Assessment
CBCT images were superimposed with the preoperative VSP using cranial base registration. Translational (x, y, z) and rotational (pitch, roll, yaw) deviations of the maxilla and mandible were measured. Clinically acceptable thresholds were ≤2 mm and ≤2°. Data were summarized as mean ± SD. Comparative statistics between sequencing groups were descriptive due to non-randomized design.
3. RESULTS
Patient Characteristics
All 46 patients completed the study. The mean age was 25.6 ± 7.2 years, with 28 females and 18 males. No intraoperative complications or conversions from PSI to splints occurred.
Maxillary Accuracy
Table 1 presents translational and rotational deviations of the maxilla. Both sequencing approaches yielded high accuracy. For mandible-first, translational deviations ranged 0.63–0.71 mm and rotational deviations 0.87–0.92°. Maxilla-first showed translational deviations 0.66–0.73 mm and rotational deviations 0.89–0.95°. These results are consistent with previously reported accuracy for PSI-guided maxillary repositioning [3,4].
| Parameter | Mandible-first (n=22) | Maxilla-first (n=24) | Literature Reference |
|---|---|---|---|
| Translation X | 0.63 ± 0.21 | 0.66 ± 0.24 | 0.5–0.8 [3,4] |
| Translation Y | 0.71 ± 0.25 | 0.73 ± 0.27 | 0.6–0.9 [3,4] |
| Translation Z | 0.68 ± 0.22 | 0.70 ± 0.23 | 0.5–0.9 [3,4] |
| Pitch | 0.87 ± 0.31 | 0.89 ± 0.32 | ~0.9 [3,4] |
| Roll | 0.92 ± 0.28 | 0.95 ± 0.29 | ≤1 [3,4] |
| Yaw | 0.88 ± 0.30 | 0.91 ± 0.31 | ≤1 [3,4] |
Table 1. Maxillary Accuracy (mean ± SD, mm / degrees)
Textual description:
Mandible-first sequencing demonstrated slightly lower anterior-posterior translation (0.63 mm vs 0.66 mm) and comparable pitch and yaw deviations. No clinically relevant differences were observed. Both sequences achieved accurate occlusal and skeletal alignment with PSI.
Mandibular Accuracy
Table 2 summarizes mandibular deviations. Mandible-first sequencing showed translational deviations of 0.72–0.81 mm and rotational deviations 0.99–1.05°. Maxilla-first sequencing showed 0.74–0.83 mm translational and 1.01–1.08° rotational deviations. These findings align with literature reporting high reproducibility of mandibular positioning using PSI [4,5].
| Parameter | Mandible-first (n=22) | Maxilla-first (n=24) | Literature Reference |
|---|---|---|---|
| Translation X | 0.72 ± 0.28 | 0.74 ± 0.29 | 0.7–0.9 [4,5] |
| Translation Y | 0.81 ± 0.33 | 0.83 ± 0.34 | 0.8–1.0 [4,5] |
| Translation Z | 0.79 ± 0.31 | 0.81 ± 0.32 | 0.8–1.2 [4,5] |
| Pitch | 1.05 ± 0.37 | 1.08 ± 0.38 | ≤1.2 [4,5] |
| Roll | 0.99 ± 0.35 | 1.01 ± 0.36 | ≤1 [4,5] |
| Yaw | 1.02 ± 0.36 | 1.05 ± 0.37 | ≤1 [4,5] |
Table 2. Mandibular Accuracy (mean ± SD, mm / degrees)
Textual description:
Mandible-first sequencing resulted in marginally lower pitch deviations (1.05° vs 1.08°) and slightly better roll alignment. Both sequences achieved accurate occlusal relationships and segment positioning. These results suggest that sequencing did not influence clinical outcomes when PSI were used.
Sequencing Comparison
No significant differences in translational or rotational accuracy were detected between mandible-first and maxilla-first sequences. Both sequences reproduced the virtual plan within clinically acceptable limits (<2 mm, <2°). Backup splints were not needed in any case, confirming the reliability of PSI.
4. DISCUSSION
The present study demonstrates that sequencing does not significantly impact surgical accuracy in PSI-guided, VSP-based bimaxillary orthognathic surgery. Both mandible-first and maxilla-first approaches reproduced planned movements with mean translational deviations <1 mm and rotational deviations <2°. This is consistent with previous reports [1–7].
Relation to Literature:
Systematic reviews and prospective studies report comparable maxillary and mandibular accuracy between sequencing strategies [1,2]. PSI significantly enhances accuracy compared to conventional splints [3,5]. Our findings align with randomized comparisons showing reliable outcomes regardless of sequencing, confirming that VSP and PSI are the primary determinants of accuracy [7].
Clinical Implications:
Sequencing should remain indication-based:
-
Mandible-first is advantageous for counter-clockwise rotation, cleft cases, and multi-segment maxillary osteotomies [6,7].
-
Maxilla-first remains appropriate for clockwise rotation or single-piece Le Fort I osteotomies [1].
PSI enables precise skeletal positioning independent of sequence. Backup splints provide safety but were unnecessary in our series.
Limitations:
-
Retrospective design and non-randomized allocation limit causal inference.
-
Single-surgeon data reduce variability but may affect generalizability.
-
Short-term postoperative CBCT (≤4 weeks) does not assess long-term skeletal stability.
5. CONCLUSION
In modern fully digital bimaxillary orthognathic surgery, surgical sequence is secondary to precise VSP and PSI-guided execution. Clinical judgment should guide sequencing decisions, while PSI ensures high surgical accuracy.
6. ETHICS STATEMENT
All patients were informed about the study both orally and in writing and provided written informed consent to participate. The study was conducted in accordance with the principles of the Declaration of Helsinki and was approved by the Ethics Committee of the Hochschule Zurich, in Zurich, Switzerland.
7. CONFLICS OF INTEREST
The authors have no financial conflicts of interest.
References
[1] Fricain M, Barthélemi S, Lapeyrie P, Masson Regnault E. Maxilla-first versus mandible-first sequencing in bimaxillary orthognathic surgery: a systematic review. J Oral Med Oral Surg. 2025;31:22.
[2] Liao YF, et al. Does surgical sequencing influence the accuracy of maxillary positioning in bimaxillary cleft orthognathic surgery? Plast Reconstr Surg. 2024; ahead of print. PMID:39046832.
[3] Accuracy of maxillary positioning using computer-designed splints or patient-specific implants in orthognathic surgery. Clin Oral Investig. 2023; ahead of print. PMID:37382718.
[4] Zhang Y, et al. Accuracy of virtual surgical planning in bimaxillary orthognathic surgery using a mandible-first sequence: a retrospective study. Plast Reconstr Surg Glob Open. 2023; ahead of print. PMID:37355372.
[5] Three-dimensional accuracy and stability of personalized implants in orthognathic surgery: a systematic review and meta-analysis. J Craniofac Surg. 2023; ahead of print. PMID:36675786.
[6] Stokbro K, et al. Accuracy assessment of mandible-first versus conventional sequencing in bimaxillary orthognathic surgery using virtual surgical planning. J Clin Med. 2023;12:6826.
[7] Single-jaw patient-specific implants in bimaxillary orthognathic surgery: a randomized comparison between maxilla-guided and mandible-guided approaches. J Craniofac Surg. 2025; ahead of print. PMID:39933970.
